Main Content
About FOR 2497: PEGASUS
Pemphigus is a rare, potentially devastating autoimmune disease of the skin and mucous membranes with high morbidity and mortality.
Based on its well-characterized immune pathogenesis, pemphigus can be considered as a paradigm of an organ-specific autoimmune disease and is used as such in the DFG Research Unit PEGASUS. The major clinical variant, pemphigus vulgaris (PV) is caused by a loss of adhesion of epidermal keratinocytes which is induced by IgG autoantibodies (auto-ab) against components of desmosomes, i.e. desmoglein 3 (Dsg3) and desmoglein 1 (Dsg1).
With PEGASUS, our consortium of basic researchers and clinician-scientists with a long-standing interest in pemphigus and immunological research will aim at dissecting key events in the immunological induction and maintenance phase of PV.
This approach will primarily focus on basic research of immunological and molecular events leading to the hallmark of PV, the loss of keratinocyte adhesion. Moreover, it has a strong translational approach with the aim to introduce therapeutic concepts originating from basic research in early phase clinical trials in PV.
Between the subprojects (TPs) of PEGASUS, our research reaches from cell biology (TP4, TP5, TP6new), immunology (TP2 and TP3), and pre-clinical mouse model (TP1) to a clinical phase 1 trial (TP8).
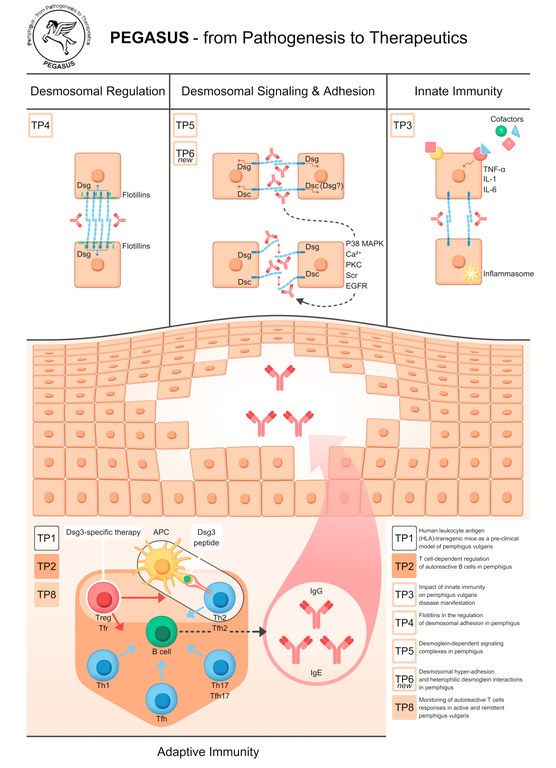
TP1: Human leukocyte antigen (HLA)-transgenic mice as a pre-clinical model of pemphigus vulgaris
TP2: T-cell-dependent regulation of autoreactive B cells in pemphigus
TP3: Innate immune responses in pemphigus vulgaris
TP4: Flotillins in the regulation of desmosomal adhesion in pemphigus
TP5: Desmoglein-dependent signaling complexes in pemphigus
TP6new: Desmosomal hyper-adhesion and heterophilic desmoglein interactions in pemphigus
TP8: Clinical phase Ib trial: T-cell-targeted immunotherapy of pemphigus vulgaris
Specifically, PEGASUS will address the following aspects of the PV pathogenesis: Utilizing a pre-clinical animal model of PV (TP1), skin biopsies and peripheral blood lymphocytes from PV patients, the relative role of autoaggressive T cells (TP1, TP2, TP8), B cells (TP2, TP4) and innate immune mechanisms (TP3) in PV will be studied in vivo/ex vivo and in vitro, respectively. Major emphasis will be also put on dissecting critical events leading to loss of epidermal adhesion by IgG auto-ab against the target antigens of pemphigus (Dsg-poteins and flotillins) (TP4, TP5). Finally, a phase I trial in PV aimed at therapeutically targeting autoaggressive T cells will translate the concept of PV as a T cell driven disorder from ex vivo and in vivo pre-clinical models into clinical reality (TP8).
Based on the broad expertise of the PEGASUS consortium, we not only expect a deepened understanding of the immunological regulation of IgG auto-ab production but also novel clues how to translate the basic research findings into clinical reality. As PV is a model autoimmune disorder, the work of the research unit PEGASUS should provide novel, more specific treatment options for auto-ab-dependent autoimmune disorders in general.





